Introduction
Several advantages of the zirconia fixed partial denture (FPD) infrastructures, such as high flexural strength and desirable optical properties with a reduced layer thickness for veneering ceramic to achieve the desired color, were reported in numerous investigators like Devigus et al. (2004), Blatz et al. (2003) and Piconi et al (1999). Besides the strength of the material, Devigus et al. (2004) and Burke et al. (2002) also reported the luting protocol as important for the clinical success. Gorodovsky and Zidan (1992) listed a variety of cements that were advised to lute zirconia FPDs; including zinc phosphate, zinc polycarboxylate, glass ionomer, urethane dimethacrylate based adhesive composite resin, Bis-GMA based composite resin, and resin modified glass ionomer cements. In ceramic restorative systems, an adhesive interface is necessary for retention. Such adhesive systems are generally based on phosphoric acid etching or self-etching techniques according to Federlin et al. (2005). Bond between the tooth and the restoration via composite resin was advised for improving retention and marginal integrity of the restorations by Behr et al. (2004), Gu and Kern (2003), Burke at al. (2002) and Rosenstiel et al. (1998). Della Bona et al. (2004,2002,2000), Ozcan (2002) and Ozcan and Valittu (2003) advocated that, surface treatment is required in order to obtain adhesion between luting agent and ceramic interface. In-vitro studies of Hoosmand et al. (2002), Jednakiewicz and Martin (2001), Barghi (2000), Kupiec et al. (1996) and Pameijer et al. (1996) have recommended the application of hydrofluoric acid (HF) followed by silane coupling agent to gain additional bond strength for the composite resin-ceramic bond. However, these studies were limited only feldspathic ceramics.
Sun et al. (2000) advised to produce a silica layer on the ceramic surface with high-speed surface impaction of alumina particles modified by silica in order to establish the chemical bond between the ceramic surface and the silane agent bonds chemically to the silica layer and to the subsequently applied composite resin. Studies of Zandparsa et al. (2014), Atsu et al. (2006), Bottino et al. (2005), Ernst et al (2005), Bo-Kyung et al. (2005), Blatz et al. (2004), Ozcan and Valittu (2003), Blatz (2002), Blixt et al. (2000) and Burke (1996) evaluated the effect of different surface treatment methods on the bond strength of resin cements to zirconia ceramics. On the other hand; Ernst et al (2005), Piwowarczyk and Lauer (2003) and Wegner and Kern (2000) examined and measured the shear bond strength of different cements on zirconium oxide ceramic surfaces after different pretreatments. Nevertheless, little information is available on the effect of non-pyrolitical tribochemical silica coating on the shear bond strength of the enamel- composite resin -zirconia joints. Therefore, the objective of this in-vitro study is to observe and compare the effect of the various adhesive luting protocols on the shear bond strengths of the enamel- composite resin-zirconia joints. The tested protocols were; silica coating and silanization of the zirconia surface prior to the luting with a methacrylate based composite resin cement, HF treatment and silanization of the zirconia surface prior to the luting with a methacrylate based composite resin cement, and luting with a methacrylate-phosphate based composite resin cement. The H0 hypothesis was constructed as: “The shear bond strength of the tested groups are indifferent”.
Material and Methods
Disc shaped (4mm in height and 4mm in diameter) 30 zirconia specimens were fabricated from yttrium-stabilized tetragonal zirconium polycrystal (Y-TZP) blanks (Cercon Smart Ceramics; Degussa Dental, Hanau, Germany), according to the manufacturer’s recommendations.
Thirty sound human molars extracted due to periodontal reasons were stored in distilled water with a few thymol crystals at room temperature until the laboratory procedures were conducted. Teeth were scaled using a hand instrument (Scaler H6/H7; Hu-Friedy, Chicago, US) and brushed (Komet GmbH, Besigheim, Germany) with non-aromatic pumice at 6000 rpm. Roots were cut off by using a double-faced diamond disc (KG Sorensen, Saõ Paolo, Brazil) under water-cooling. Flat enamel surfaces, 4mm in diameter were prepared on the buccal surfaces of each tooth specimen by using a high-speed diamond wheel (057 524, Intensiv SA, Lugano, Switzerland) under water-cooling. Crowns of each tooth were then embedded in auto-polymerizing acrylic resin (Imicryl SC, Imicryl Diş Malz. San. Tic. A.Ş., Konya, Turkey) in plastic cylindrical molds in order to hold the prepared enamel surface exposed in the middle of the circular face of the acrylic resin base. Acrylic resin bases were then allowed to polymerization for 30 minutes and afterwards removed from the plastic molds and kept in distilled water.
In Group HF, the luting surface of the zirconia disc was treated with 9.5% HF (Porcelain Etch, Ultradent, Utah, US) for 40 seconds then rinsed and air-dried. Wetted with a silane coupling agent (Silane, Ultradent) and allowed to evaporate for 5 minutes.
Prepared enamel surfaces were etched with 37% orthophosphoric acid (Email Preparator, Ivoclar-Vivadent, Schaan, Liechtenstein) for 30 seconds, rinsed and air-dried. Syntac Adhesive (Ivoclar-Vivadent) was applied for 10 seconds and then air-dried. Bonding agent (Heliobond, Ivoclar-Vivadent) was applied both on enamel and zirconia surfaces but not light polymerized, protected from environmental light under a black cover. A low viscosity dual-cure methacrylate based composite resin luting agent (Variolink II, Ivoclar-Vivadent) was mixed according to the manufacturer’s recommendations, loaded on the luting surface of the zirconia disc, seated, and a standard weight of 500 grams was applied. The excess cement was removed, and the specimens were light-polimerized with an energy density of 480mW/cm2 (Bluephase C8, Ivoclar-Vivadent) for 40 seconds on each quarter of the block to a total of 160 seconds. Weight was held in position for 10 minutes on the cemented specimens.
In Group SC, the luting surface of the zirconia disc was silica coated with 30 µm alumina particles treated with silisic acid (CoJet Sand, 3M-ESPE), by using a non-pirolitical airborne-particle blaster (CoJet Particle Microblaster, 3M-ESPE). The coating procedure was performed perpendicular to the zirconia surface at 10mm distance under 3 bars of pressure for 15 seconds and then a silane coupling agent (Silane, Ultradent) was applied and allowed to dry for 5 minutes. Teeth surfaces were treated and pretreated zirconia surfaces were luted to prepared tooth surfaces and light-polymerized as described in Group HF.
In Group PF, equal amounts of Primer II A and B (ED Primer, Kuraray Co Ltd, Okayama, Japan) were mixed, applied on the prepared tooth surface for 30 seconds and air-dried gently. Equal amounts of A and B pastes of a methacrylate-phosphate based dual-cure adhesive resin cement (Panavia F, Kuraray Co. Ltd.) were mixed according to the manufacturer’s instructions, loaded on the zirconia disc, placed and a standard weight of 500 gms was applied. The excess cement was removed, a polyvinyl alcohol gel (Oxyguard; Kuraray Co) was applied on the marginally exposing cement-line, and the restorations were light-polimerized. Weight was held in position for 10 minutes on the cemented specimens.
Cemented specimens were washed with a dental unit air-water spray and stored in distilled water at room temperature for 24 hours prior to thermal cycling. Afterwards, they were thermo-cycled between water temperatures of 5 o C and 55 o C for 5000 cycles with a 15-second dwell time at each temperature.
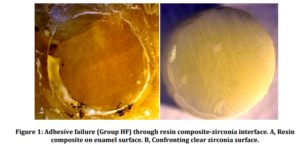
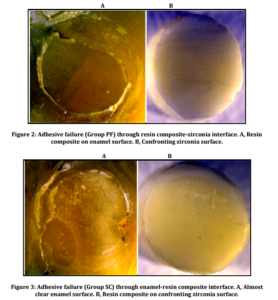
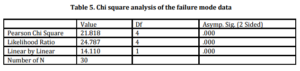
Specimens were shear-loaded to failure with a universal testing machine (KgN 50, Shimadzu Corp., Kyoto, Japan) at a crosshead speed of 0.5 mm/min. The shear bond strength values were recorded in megapascals. Data were analyzed statistically by one way analysis of variance (ANOVA) and post-hoc multiple comparisons were made with Dunnett-T3 test. Fractured surfaces of the failed specimens were also observed by a stereomicroscope (Leica Microsystems DMI 6000, Heerbrugg, Switzerland); failure modes were recorded and the data were analyzed statistically by the chi-square test. Selected surfaces from failed specimens were also inspected under scanning electron microscope (SEM) (JSM-5200, JEOL, Kyoto, Japan) and the photomicrographs were taken.
Results
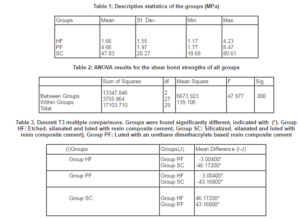
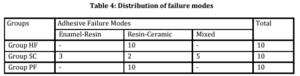
The descriptive statistics of the groups are listed in Table 1. Table 2 presents the results of the ANOVA which revealed the shear bond strengths differed significantly between all groups (P=.00) and H0 hypothesis was rejected. Post-hoc multiple comparisons computed with Dunnett T3 multiple range test and results are listed in Table 3. The highest shear bond strength of 47.8 ± 20.2 MPa was obtained from Group SC. The shear bond strength values were significantly higher for Group SC; in comparison with Group HF (1.6 ± 1.5 MPa) and also Group PF (4.6 ± 1.9 MPa) (P<.05). Group HF exhibited the lowest shear bond strength value.
The statistical analysis of the present study revealed significant differences between the mean shear bond strength values among the tested groups. The mean shear bond strength value of Group SC was found significantly higher than remaining. This finding confirms the increasing effect of the silica coating and silanization on the bond strength between enamel, composite resin and zirconia. Della Bona et al. (2000, 2002, 2004), Ozcan and Valittu (2003) and Ozcan (2002) advocated that silica coating procedure creates a fine rough surface increasing the surface area and, thus, enhances the mechanical and chemical bonding. Studies of Bo-Kyoung et al. (2005), Ozcan and Valittu (2003), Ozcan (2002) and Sun et al. (2000) reported that, silica layer on the ceramic surface processed with high-speed surface impaction of alumina particles modified by silica, forming a chemical bond between the ceramic surface and the silane agent and the silane bonds chemically to the silica layer and to the subsequently applied composite resin. Bottino et al. (2005) and Sun et al. (2000) reported that, most silane coupling agents also increase the substrate surface energy and improve the surface wettability to resins. The results of the present study are in accordance with those of Atsu et al. (2006) and Bottino et al. (2005) who reported that the silica coating followed by silanization increased the bond strength between airborne particle abraded zirconium oxide ceramic and methacrylate-phosphate based resin composite. In contrast with the results of the present study, Wegner et al. (2000) reported that higher resin bond strength to zirconium-oxide ceramic was obtained from the airborne-particle abraded zirconium-oxide ceramic specimens, while silica coated specimens were failing. Zandparsa et al. (2014) found the mean shear bond strength of the silica coated zirconia specimens to be stronger than the groups of abraded with airborne-particles, primed with alloy primer and etched with phosphoric acid; but weaker than the group of the specimens primed with zirconia primer.
The microporosities originating from the surface treatment methods are known as crack initiators and therefore weaken the ceramic material according to Blatz (2002) and Blatz et al. (2003). However, it has been known that resin luting agents significantly strengthen ceramic materials by healing the minor surface cracks since the studies of Burke et al. (2002) and Burke (1996). Mechanical retention performed with surface roughening and chemical retention with a silane coupling agent is essential to obtain reliable bond strength between composite resin and ceramic materials. For high-strength ceramics, acid etching had less effect on providing reliable bond strength between composite resin and ceramic materials according to the reports of Kupiec et al. (1996), Pameijer et al. (1996).
In the present study, the group of the specimens etched with hydrofluoric acid demonstrated significantly lower shear bond strength values in comparison with remaining groups. Higher shear bond strength values obtained from the silica coated group (Group SC) can be explained by the increased surface roughness and increased silica content resulting from the silica coating which is previously advocated by Sun et al. (2000).
Ozcan (2002) reported that, acids etch mainly the glassy phase, removing some silica from the surface to create a retentive topography for micromechanical bonding. Similar studies such as Hoosmand et al. (2002) and Jedinakiewicz and Martin (2001) scooped on the acid-resistant ceramics reported higher bond strength values when a MDP containing dual cure adhesive resin luting agent was used. However, the present study reveals that the shear bond strength obtained from Group SC was higher than the group PF, and the difference was found statistically significant.
Despite the fact that Y-TZP FPDs may be luted conventionally as recommended by manufacturers; adhesive cementation should preferred since resin cements provided improved marginal seal for all ceramic restorations according to Behr et al. (2004) and Gu and Kern (2003)’s studies. Some additional techniques are required to increase the bond strength of resin composite cements to acid-resistant ceramics. Regarding the bonding mechanism between the composite resin and zirconia, silica coating and silanization can enhance the mechanical bond strength of ceramic materials to the composite resin. Ernst et al. (2005) compared the bonding performance of conventional and composite resin cements and reported that only a few of them demonstrated significantly higher median retentive strength values than a glass ionomer and a resin modified glass ionomer cement while the retentive strength did not profit significantly from a non-pirolitical silica coating pretreatment (Rocatec) for the zirconia crowns. The non-pirolitical silica coating pretreatment of the zirconia crowns resulted in an increase of median retentive strength values of more than 50%, but did not prove to be statistically significant. These results are not in accordance with the results of the present paper that confirms that the non-pirolitical tribochemical silica coating increased the bond strength of the zirconia to adhesive resin and found to be statistically significant.
Results of the present study demonstrated that, Group PF showed higher shear bond strength values than Group HF and the difference was found to be significant (P<.05). Piwowarczyk et al. (2003) used a representative of an adhesive composite resin that was developed with the goal of combining the ease of handling and absence of required pretreatment steps, with firm adhesion to tooth structure, demonstrated high shear bond strength to zirconia under specific conditions. Blatz et al. (2004) evaluated and compared resin bond strength before and after artificial aging (long term storage and thermal cycling) to airborne—particle-abraded Procera AllZirkon ceramic with a phosphate-monomer (MDP) containing bonding/silane coupling agent. The authors showed that silane coupling agent containing an adhesive phosphate monomer can achieve superior long-term shear bond strength to airborne—particle—abraded Procera AllZirkon restorations while artificial aging significantly reduced bond strength. Mechanical and chemical aging are the factors that can have effects on the durability of the resin bond strength to zirconia, and they are important parameters to simulate oral conditions. In the present study, the effects of chemical and mechanical aging on the bond strength were not evaluated. The type of adhesive resin cements also influence the shear bond strength values but this was discarded in this study in order to prevent confusion due to the increase in the number of variables. In addition, the present study scooped to the shear bond strength obtained from the enamel tissue. However, enamel tissue is only one of the hard tooth tissues. Shear bond strengths of the zirconia—composite resin-dentine joints should also be inspected. These factors may be considered within the limitations of this study.
Bottino et al. (2005) showed that, tribochemical silica coating might increase the bond strength between composite resin and high-strength ceramics. Similarly, Blixt (2000) reported that, tribochemical silica coating (Rocatec) provides durable resin bonds to glass-infiltrated aluminum oxide ceramics with Bis-GMA-based composite resin cements. An advantage of this system is that silica coating units are available for use in both the dental laboratory and dental office. In the present study, a chair-side microblaster (CoJet Particle Microblaster) was employed. The results of the present study showed that tribochemical treatment followed by silanization improved bond strength with composite resin. Blixt (2000) explained this increase by 2 different mechanisms. First, microscopic irregularities created by the 100 µm aluminum oxide silica-coated airborne-particle abrasion may provide mechanical retention. The second mechanism relies on a special coating generated by the adhesive layer of silica followed by the silane application. By this mechanism, the SiO2 is tribochemically transformed and is consequently able to bond to metal alloys and high-density ceramics.
Hooshmand et al. (2002) analyzed the role of a heat treatment following the application of silane on the bond strength between composite resin and feldspathic ceramics. Authors found that the composite resin bond to a ceramic surface, in the group that received a heat treatment after silane application, was as good as the bond to ceramic groups in which surface treatments included micromechanical retention provided by airborne-particle abrasion or hydrofluoric acid etching.
Conclusions
Within the limitations of this study, the following conclusions were drawn:
1. The shear bond strength values were found significantly different among the groups tested. Specimens that luted with urethane dimethacrylate based adhesive cement showed higher bond strength values than the specimens of acid etched, silanated and luted with resin composite cement (P<.05); but lower bond strength values, in comparison with the specimens of silica coated, silanized and luted with composite resin cement.
2. The tested non-pirolitic tribochemical silica coating system (CoJet) significantly increased (P<.05) the shear bond strength between Y-TZP based ceramics and adhesive resin cement. The specimens silica, coated and silanized prior to luted with composite resin cement, showed the highest shear bond strength values.
References
1. Atsu SS, Kilicarslan MA, Kucukesmen HC, Aka PS. Effect of zirconium-oxide ceramic surface treatments on the bond strength to adhesive resin. J Prosthet Dent 2006;95:430-6
2. Behr M, Rosentritt M, Regnet T, Lang R, Handel G. Marginal adaptation in dentin of a self-adhesive universal resin cement compared with well-tried systems. Dent Mater 2004;20:191-7
3. Blatz MB, Sadan A, Kern M. Resin-ceramic bonding: a review of the literature. J Prosthet Dent 2003;89:268-74
4. Blatz MB, Sadan A, Martin J, Lang B. In vitro evaluation of shear bond strengths of resin to densely-sintered high-purity zirconium oxide after long-term storage and thermal cycling. J Prosthet Dent 2004;91: 356-62
5. Blatz MB. Long-term clinical success of all ceramic posterior restorations. Quintessence Int 2002;3:415-26
6. Blixt M, Adamczak E, Linden L, Oden A, Arvidson K. Bonding to densely sintered alumina surfaces: effect of sandblasting and silica coating on shear bond strength of luting cements. Int J Prosthodont 2000; 13:221-6
7. Bo-Kyoung K, Bae HE, Shim JS, Lee KW. The influence of ceramic surface treatments on the tensile bond strength of composite resin to all ceramic coping materials. J Prosthet Dent 2005;94:357-62
8. Bottino MA, Valandro LF, Scotti R, Buso L. Effect of surface treatments on the resin bond to zirconium-based ceramic. Int J Prosthodont 2005;18: 60-5
9. Burke FJ, Fleming GJ, Nathanson D, Marquis PM. Are adhesive technologies needed to support ceramics? An assessment of the current evidence. J Adhesive Dent 2002;4:7-22
10. Burke FJ. Fracture resistance of teeth restored with dentin-bonded crowns: the effect of increased tooth preparation. Quintessence Int 1996;27:115-21
11. Della Bona A, Anusavice KJ, Hood JA. Effect of ceramic surface treatment on tensile bond strength to a resin cement. Int J Prosthodont 2002;15: 248-53
12. Della Bona A, Anusavice KJ, Shen C. Microtensile strength of composite bonded to hot-pressed ceramics. J Adhesive Dent 2000;2:305-13
13. Della Bona A, Shen C, Anusavice KJ. Work of adhesion of resin on treated lithia disilicate-based ceramic. Dent Mater 2004;20:338-44
14. Devigus A, Lombardi G. Shading Vita In-ceram YZ substructures: influence on value and chroma, part II. Int J Comput Dent 2004;7:379-88
15. Ernst CP, Cohnen U, Stender E, Willershausen B. In vitro retentive strength of zirconium oxide ceramic crowns using different luting agents. J Prosthet Dent 2005;93:551-8
16. Federlin M, Sipos C, Hiller KA, Thonemann B, Schmalz G. Partial ceramic crowns. Influence of preparation design and luting material on margin integrity— a scanning electron microscopic study. Clin Oral Investig 2005;9:8-17
17. Gorodovsky S, Zidan O. Retentive strength, disintegration, and marginal quality of luting cements. J Prosthet Dent 1992;68:269-74
18. Gu XH, Kern M. Marginal discrepancies and leakage of all-ceramic crowns: influence of luting agents and aging conditions. Int J Prosthodont 2003;16:109-16
19. Hooshmand T, van Noort R, Keshvad A. Bond durability of the resinbonded and silane treated ceramic surface. Dent Mater 2002;18:179-88
20. Jedynakiewicz NM, Martin N. The effect of surface coating on the bond strength of machinable ceramics. Biomaterials 2001;22:749-52
21. Kupiec KA, Wuertz KM, Barkmeier WW, Wilwerding TM. Evaluation of porcelain surface treatments and agents for composite-to-porcelain repair. J Prosthet Dent 1996;76:119-24
22. Ozcan M, Vallittu PK. Effect of surface conditioning methods on the bond strength of luting cement to ceramics. Dent Mater 2003;19:725-31
23. Ozcan M. The use of chairside silica coating for different dental applications: a clinical report. J Prosthet Dent 2002;87:469-72
24. Pameijer CH, Louw NP, Fischer D. Repairing fractured porcelain: how surface preparation affects shear force resistance. J Amer Dent Assoc 1996; 127:203-9
25. Piconi C, Maccauro G. Zirconia as a ceramic biomaterial. Biomaterials 1999;20:1-25
26. Piwowarczyk A, Lauer HC. Mechanical properties of luting cements after water storage. Oper Dent 2003;28:535-42
27. Rosenstiel SF, Land MF, Crispin BJ. Dental luting agents: a review of the current literature. J Prosthet Dent 1998;80:280-301
28. Sun R, Suansuwan N, Kilpatrick N, Swain M. Characterisation of tribochemically assisted bonding of composite resin to porcelain and metal. J Dent 2000;28:441-5
29. Wegner SM, Kern M. Long-term resin bond strength to zirconia ceramic. J Adhesive Dent 2000;2:139-47
30. Zandparsa R1, Talua NA, Finkelman MD, Schaus SE. An in vitro comparison of shear bond strength of zirconia to enamel using different surface treatments. J Prosthodont 2014 23:117-23