Introduction
The deformation and aggregation properties of the erythrocytes as the most abundant blood cells play a crucial role in maintaining normal bloodstream. The increase of the erythrocyte aggregation and reduction of the deformability with strengthening of blood viscosity has been demonstrated in patients with coronary heart diseases (Koenig, Ernst, 1992;Leschke, 2008; Santos et al., 2011). Nonetheless, the contribution of hemorheological alterations in the prothrombotic condition in patients with atherosclerosis remains a question of debate. We aimed to determine the association between lipid spectrum of the blood plasma and hemorheological parameters.
Materials and Methods
In the study we compared blood lipid levels in chronic patients with typical stable angina. The investigation deals with the whole blood obtained from 49 patients (men 58-74 years), chronically suffering from angina of II, III and IV functional class in the morning before a meal and drug therapy in the clinic during a periodic inspection. The systolic or diastolic blood pressure was ≥140 mm Hg or 90 mm Hg. All the patients gave a written informed consent and approved the study protocol. Heparin in concentration of 100 units/ml was used as anticoagulant. Experiments were undertaken with the understanding and verbal consent of each subject according to the conditions set forth by a Human Subjects and Ethics Review Board. The study conforms with the Code of Ethics of the World Medical Association (Declaration of Helsinki).
The reversible tendency to form an aggregates (REA) was determined by Tukhvatulin et al (1986) in our modification (Katiukhin, 2013) from analyzing the light transmission data through the whole heparinized blood samples at hematocrit 40% in a glass micro-chamber of 25 mcm height and of 16 mm diameter. The full erythrocyte disaggregation shear stress is achieved by voltage increase on piezo-crystal connected with the surface of the micro-chamber. The time of full disaggregation was interpreted as the maximum strength of erythrocyte aggregates (Tfull). The rate of spontaneous aggregation (K) was determined from a half-period reduction of the photometric transient signal through completely disaggregated blood after power-down. The integral index of aggregation (Iaggr) was calculated as (Tfull x K). The deformability of erythrocytes (ED) was studied using the method of gradient ektacytometry by Johnson (1989). Data from lipid profiles included total cholesterol (CHOL), triglycerides (TG), low-density lipoprotein (LDL) and high-density lipoprotein (HDL) levels. CHOL, TG and HDL concentrations were measured by a standard semi automatic method using Technicon-AA-2 unit (USA), content of LDL was calculated by Friedwald et al (1972). The atherogenic index (Iatherog) was calculated as (CHOL — HDL)/ HDL. All measurements were done at constant temperature of 25°C. The results were expressed as the means ± SD. Student’s unpaired t-test was used to compare the data. Statistical significance was declared when P<0.05.
Results
The patients were divided into groups according to CHOL content (less than 200, 200 -239 or more 239 mg/dl), LDL (less than 130, 130 -159 or more 159 mg/dl), HDL (more than 49, 49 – 35 or less 35 mg/dl) and TG (less or more than 200 mg/dl). The results are shown in Table 1.
Table 1: Rheological Properties of Red Blood Cells Depending on the Level of Lipids
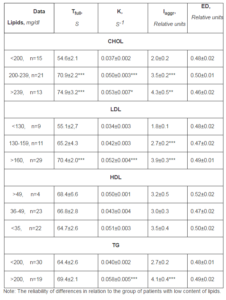
It can be seen that the higher the concentrations LDL and CHOL, the more K, Tfull and Iaggr will be. When the concentration of TG increased, K was raised only without significant increase in Tfull. Noteworthy is the fact that the rheological properties of erythrocytes did not change depending on the HDL. The correlation analysis confirms this. Thus, the CHOL and LDL positively correlated with Tfull. (r = 0.49 and 0.40, respectively, p<0.0004), with K (r = 0.45 and 0.51 respectively, p<0.001) and with Iaggr (r = 0.69, p<0.0001 in both cases). TG concentration in plasma was positively correlated with K and Iaggr (r = 0.41 and 0.43 respectively, p<0.003). HDL was not associated with the rheological parameters of erythrocytes.
We conducted more detailed analysis dividing all patients into 3 groups with lipid levels, corresponding to normal (less than 3), moderately increased (from 3 to 4) and the high value of atherogenic index (Iatherog) (Table 2). Each group was allocated to three subgroups characterized by the following values of REA: group 1 – K less than 0,045 S-1, Tfull less than 53 S and Iaggr less than 3.1 relative units; group 2 – respectively (0, 045-0,050) S-1, (53-62) S and (3.1-3.5) relative units; group 3 – respectively over 0, 050 S-1, over 62 S and over 3.5 relative units (Table 3). The overall picture of the aggregation parameters of erythrocytes in patients depending on the level of lipids is shown in Figure 1.
Table 2: Lipid Concentrations Corresponding to the Normal, Moderately Increased and High Values of Atherogenic Index
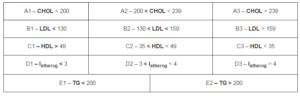

Table 3: Lipid Subgroups Corresponding to Low, Medium and High Values of Aggregation
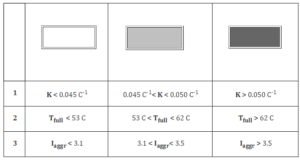
As the figure shows, among patients with high CHOL (group A) and LDL (group B) the percentage of patients with enhanced REA is higher than among patients with low levels of these lipids. A similar pattern is observed in groups D and E (Iatherog and TG). The distribution pattern of indicators REA in the subgroup with different HDL (group C) shows that the content of HDL is not reflected on erythrocyte aggregation. The analysis showed that the deformation properties of red blood cells were not associated with the plasma lipid profile.
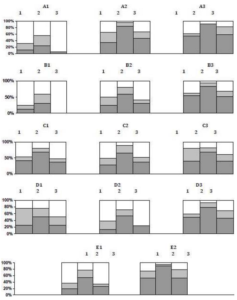
Figure 1: The Reversible tendency of RBC to Form Aggregates Depending on the Level of Lipids in the Blood
Discussion
According to the modern concepts in hematology, the mammalian blood is a structure similar to the gel where aggregates of red blood cells can break and be formed again. Therefore, the aggregation and deformation of erythrocytes as the most abundant blood cell abilities have a leading importance for this process and play a crucial role in maintaining normal bloodstream structure. Many researchers have viewed the low high-density lipoprotein cholesterol (HDL) as a risk factor for growth of atherosclerotic cardiovascular disease (Moriarty, Gibson, 2005; Subedi et al., 2014). Modern medicine has used the increased level of HDL like an attractive strategy of treatment, but there are no clear guidelines for such treatment due to the lack of solid outcomes data for HDL specific therapies. In conclusion, no relation was found between content of high density lipoproteins and the erythrocyte’s aggregation, while aggregation increased with increasing concentration of low-density lipoproteins in the blood. Known anti-atherogenic properties of this class lipoproteins apparently did not related to their effect on blood rheology.
References
1.Friedwald, W. T., Levy, R. I. & Fredrickson, D. S. (1972). ‘Estimation of the Concentration of Low Density Lipoprotein Cholesterol in Plasma without Use of Preparative Ultracentrifuge,’ Clinical Chemistry, 18 (6) 499-502.
2.Johnson, R. M. (1989). “Ektacytometry of Red Blood Cells,” Methods in Enzymology, 173 (Pt.T) 35-54.
Publisher – Google Scholar
3.Katiukhin, L. N. (2013). “Erythrocyte Shape Transformation in Physiological Regulation of Blood Viscosity,” Open Journal of Molecular and Integrative Physiology, 3(4) 194-198.
Publisher – Google Scholar
4.Koenig, W. & Ernst, E. (1992). “The Possible Role of Hemorheology in Atherothrombogenesis,” Atherosclerosis, 94(2-3) 93-107.
Publisher – Google Scholar
5.Leschke, M. (2008). “Rheology and Coronary Heart Disease,” Deutsche Medizinische Wochenschrift, 133(Suppl 8) 270-273.
Publisher – Google Scholar
6.Moriarty, P. M. & Gibson, C. A. (2005). “Association between Hematological Parameters and High-Density Lipoprotein Cholesterol,” Current Opinion in Cardiology, 20(4):318-323.
Publisher – Google Scholar
7.Santos, M. J., Pedro, L. M., Canhão, H., Fernandes, J. F., Canas da Silva, J., Fonseca, J. E. & Saldanha, C. (2011). “Hemorheological Parameters are Related to Subclinical Atherosclerosis in Systemic Lupus Erythematosus and Rheumatoid Arthritis Patients,” Atherosclerosis, 219(2)821-6.
Publisher – Google Scholar
8.Subedi, B. H., Joshi, P. H., Jones, S. R., Martin, S. S., Blaha, M. J. & Michos, E. D. (2014). “Current Guidelines for High-Density Lipoprotein Cholesterol in Therapy and Future Directions,” Vascular Health and Risk Management, 8(10):205-216.
Publisher – Google Scholar
9.Tukhvatulin, R. T., Levtov, V. A., Shuvaeva, V. N. & Shadrina, N. Kh. (1986). “Aggregation of Erythrocytes Placed in Macro- and Micro-Cuvettes,” Fiziologicheskii Zhurnal SSSR Imeni I. M. Sechenova, 72(6) 775-784.
Publisher – Google Scholar







