It is widely recognized that the balance of forces on the teeth from the lips and tongue is one of the most important factors determining the position of the dental arch (Ahlgren JG et al., 1973, Lowe AA et al., 1984, Jung MH et al., 2003). In other words, lip force can affect craniofacial morphology. This was proposed in the 1950s as the buccinator mechanism in orthodontics (Brodie AG., 1953, Moyers RE., 1958). The effects of lip-closing force (LCF) on dentition have been applied for orthodontic treatments such as myofunctional therapy.
Many studies have attempted to clarify the relationship between the LCF of subjects and their malocclusion using various systems for measuring LCF. For example, by using a dynamometer, LCF was measured as vertical lip force for upper and lower lips, the same as with the Myometer 160 (Ingervall B et al., 1981, Posen AL., 1976, Lambrechts H et al., 2010). Another measurement system involved the lip pressure on the incisors (Thuer U et al., 1986). Jung et al., (2003 and 2010) attempted to measure the upper- and lower-lip forces separately using a Y-meter. However, these studies did not obtain consistent findings on the relationship between LCF and malocclusion because of the different measurement methods and developmental stages of subjects.
The orbicularis oris muscle (OOM), which plays a dominant role in producing LCF, is an orbicular muscle surrounding the oral slit and does not function in a simple manner. It is innervated by the facial nerve, mainly unilaterally. In addition, it is comprised of two different components: one is the buccal branch in the upper labial part and the other is the mandibular branch in the lower labial part. In addition, the upper and lower parts of the OOM have different functional properties in force development, stability and fatigability (Amerman JD., 1993, Barlow SM et al., 1996, Gentil M et al., 1998).
These characteristics of the OOM enable various patterns of LCF to be performed, corresponding to particular functions. It is thought that, when we maintain static force control of the lips, the multidirectional outputs of LCF can be controlled by precise cooperation between numerous contacts surrounding the lips. From this perspective, the balance of different directional LCF may affect the morphology.
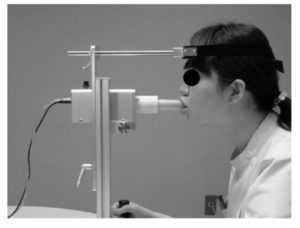
We have developed a multidirectional LCF measurement system that allows us to measure the LCF in eight different directions during pursing-like lip-closing (Nakatsuka K et al., 2011a), and we reported the properties of multidirectional LCF for healthy young adults, as well as postoperative patients with cleft lip and/or palate (Nakatsuka K et al., 2011abc, Murakami M et al., 2012). We demonstrated the ability to analyze the directional balance of LCF using multidirectional LCF.
Alteration of the dental axis was shown to compensate for the occlusal function when the anterior-posterior position between maxillary and mandibular regions is incorrect skeletally. This phenomenon called “dental compensation” has been frequently observed in clinical dentistry. However, the mechanism that causes it has remained unclear.
We hypothesized that an imbalance in upper and lower lip forces affecting teeth position and/or inclination does not result in malocclusion, but rather in dental compensation, in young adults with skeletal malocclusion at a late stage of development. The aim of this study was to test this hypothesis by measuring multidirectional LCF during pursing-like lip-closing and lateral craniofacial morphology.
Materials and Methods
Subjects
This research was approved by the Ethics Committee on Clinical Research of Matsumoto Dental University (Approval Number: 0057). Sixty-two females (median = 23.0 years, range = 17—34 years) were recruited from among patients with malocclusion who were referred to the Department of Orthodontics of Matsumoto Dental University Hospital. None had a history of lip injury or neurological disease. This study excluded those with a remarkable lateral shift of the mandible (magnitude of shift of the menton larger than 4.0 mm on a frontal cephalogram), those with previous experience of orthodontic treatment and those with missing teeth, including the congenital lack of teeth (apart from third molars). All subjects received verbal and written information about the study and gave verbal consent to participate.
Classification of subjects
In all subjects, standardized lateral cephalometric radiographs were taken with the lips closed and centric occlusion. From their lateral cephalograms, the subjects were divided into 3 groups (skeletal Classes I, II and III) using the value of ANB as follows:
(1) skeletal Class I: ANB 2°—4°;
(2) skeletal Class II: ANB>4°;
(3) skeletal Class III: ANB<2°.
Analysis of lateral cephalogram
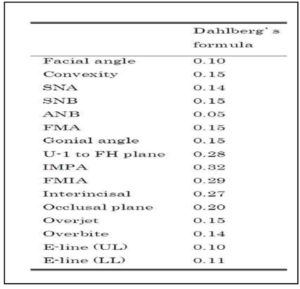
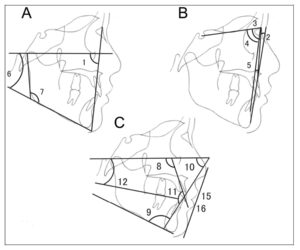
Skeletal, dental and soft-tissue cephalometric landmarks were determined using software (Win Ceph® version 9.0, Rise Co., Miyagi, Japan). In order to determine the characteristics of the facial skeleton and the inclination of anterior teeth, we measured 11 angles and 4 lengths from the reference points and lines of the lateral cephalogram (Fig. 1).
In order to determine the measurement error, cephalograms of ten subjects chosen at random were traced twice at an interval of two weeks and the error was calculated using Dahlberg’s formula (Dahlberg G., 1940).
Discussion
TLCF
Many previous studies showed the relationship between Angle classification and lip force. Posen (1976) measured high lip strength with maximum voluntary contraction using a pommeter (perioral muscle meter). Lip pressure on the incisors of subjects with Angle Class II div. 2 was high, and that on the incisors of subjects with Angle Class II div. 1 was lower than those with Angle Class I. Lambrechts et al., (2010) also obtained the same results using Myometer 160, which measured the LCF generated between upper and lower lips at the midline during lip-closing.
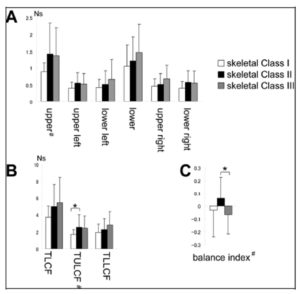
Those studies assessed lip force generated by the whole lip. Therefore, we accessed total LCF, namely, the sum of 8 directional LCF during pursing-like lip-closing, for comparison with these previous results. TLCF did not differ among skeletal Classes I, II and III in this study. This may have depended on the different classifications by skeletal pattern. U1 to FH of subjects with skeletal Class II in this study ranged from 81.0° to 131.7°. This means that skeletal Class II in our study might include both Angle Class II div. 1 and 2.
The previous results showing that the lip force of subjects with Angle Class II div. 1 was weaker and that of subjects with Angle Class II div. 2 was greater may be related to the angulation of upper incisors in previous studies, but not the skeletal pattern.
Upper- and lower-lip forces
The results obtained using a Y-meter showed the upper-and lower-lip forces separately. Therefore, by our methods, TULCF and TLLCF, namely, the sums of the 3 upper and 3 lower DLCFs, respectively, were used for upper- and lower-lip forces for comparison with the results obtained using a Y-meter. The TULCF in skeletal Class II was greater than that in skeletal Class I. This result is similar to previous results of lip pressure on the upper incisors in children (Thuer U et al., 1986). The lip pressure on the upper incisors was higher in Angle Class II div. 1 than in Angle Class I. These findings suggest that the pressure from the lips on the teeth may cause lingual angulation of the upper incisors in children. This incisor angulation may be involved in dental compensation in adults. The same study showed that the lip pressure on the upper incisors was lowest in Angle Class II div. 2 in children. This seemed to show that our subjects in skeletal Class II tended not to have incisors with lingual angulation. Indeed, the mean of the U1-FH plane angle was 107.8° in our skeletal Class II subjects, which is within the normal range.
Balance of upper and lower LCF
For the purpose of this study, we classified the subjects as having a skeletal pattern of dental compensation for those with skeletal malocclusion. In this study, upper- and lower-lip forces were estimated using the balance of upper and lower LCF.
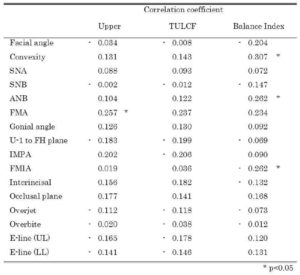
This study revealed that the balance index of upper and lower LCF showed positive correlations with ANB and convexity, and a negative correlation with FMIA. In short, in subjects of skeletal Class II, in which mandibular bone is positioned posterior to maxillary bone, upper-lip force is greater than lower-lip force, and this balance of lip force is considered to cause labial inclination of the lower incisors. In subjects of skeletal Class III, in which mandibular bone is positioned anterior to maxillary bone, lower-lip force is greater than upper-lip force, and this balance of lip force is considered to cause lingual inclination of the lower incisors. These findings support the concept of dental compensation, that is, compensation for the anterior-posterior malposition of the maxillary and mandibular regions by inclination of the incisors. The other result of the total upper LCF in group II being significantly greater than that in the other groups also supports the concept of dental compensation.
In order to prevent relapse, it is necessary to determine the muscle forces of soft tissues in the preoperative period. This study suggests that muscle activity can cause dental compensation and may provide useful information for orthodontic treatment, including the prevention of relapse.
Conclusions
There were weak positive correlations between upper LCF and FMA, and the balance index of upper and lower LCF and ANB or convexity. In addition, there was a negative correlation between FMIA and the balance index of upper and lower LCF. These findings support the concept of dental compensation, that is, compensation of the anterior-posterior malposition of the maxillary and mandibular regions by inclination of the incisors.
References
1. Ahlgren, J. G., Ingervall, B. F. and Thilander, B. L. (1973) “Muscle activity in normal and postnormal occlusion,” American Journal of Orthodontics, 64 (5) 445-456.
Publisher – Google Scholar
2. Amerman, J. D. (1993) “A maximum-force-dependent protocol for assessing labial force control,” Journal of Speech and Hearing Resarch, 36 (3) 460-465.
Google Scholar
3. Barlow, S. M. and Bradford, P. T. (1996) “Comparison of perioral reflex modulation in the upper and lower lip, ” Journal of Speech and Hearing Research, 39 (1) 55-75.
Google Scholar
4. Brodie, A. G. (1953) “Muscular Factors in the Diagnosis and Treatment of Malocclusions,” Angle Orthod, 23 (4) 71-77.
Google Scholar
5. Dahlberg, G. (1940) Satistical methods for medical and biological students, Interscience Publications, New York, USA.
6. Gentil, M. and Tournier, C. L. (1998) “Differences in fine control of forces generated by the tongue, lips and fingers in humans,” Archives of Oral Biology. 43 (7) 517-523.
Publisher – Google Scholar
7. Houston, W. J. B. (1983) “The analysis of errors in orthodontic measurements,”American Journal of Orthodontics. 83 (5) 382—390
Publisher – Google Scholar
8. Ingervall, B. and Janson, T. (1981) “The value of clinical lip strength measurements,” American Journal of Orthodontics. 80 (5) 496-507.
Publisher – Google Scholar
9. Jung, M. H., Yang, W. S. and Nahm, D. S. (2003) “Effects of upper lip closing force on craniofacial structures,” American Journal of Orthodontics and Dentofacial Orthopedics. 123 (1) 58-63.
Publisher – Google Scholar
10. Jung, M.H.,Yang, W.S. and Nahm, D.S. (2010) “Maximum Closing Force of Mentolabial Muscles and Type of Malocclusion,” Angle Orthod. 80 (1) 72-79.
Publisher – Google Scholar
11. Lambrechts, H., Baets, E. D., Fiews, S. and Willems, G. (2010) “Lip and tongue pressure in orthodontic patients,” European Journal of Orthodontics. 32 (1) 466-471.
Publisher – Google Scholar
12. Lowe, A. A. and Takada, K. (1984) “Associations between anterior temporal, masseter, and orbicularis oris muscle activity and craniofacial morphology in children,” American Journal of Orthodontics. 86 (4) 319-330.
Publisher – Google Scholar
13. Moyers, R. E. (1958) Handbook of Orthodontics, The Year Book Publishers, Chicago, USA.
14. Murakami, M., Adachi, T., Nakatsuka, K., Kato, T., Oishi, M. and Masuda, Y. (2012) “Gender differences in maximum voluntary lip-closing force during lip pursing in healthy young adults, ” Journal of Oral Rehabilitation. 39 (6) 399-404.
Publisher – Google Scholar
15. Nakatsuka, K., Adachi, T., Kato, T., Oishi, M., Murakami, M., Okada, Y. and Masuda, Y. (2011a) “Reliability of novel multidirectional lip-closing forcemeasurement system,” Journal of Oral Rehabilitation. 38 (1) 18-26.
Publisher – Google Scholar
16. Nakatsuka, K., Adachi, T., Kato, T., Oishi, M. and Masuda, Y. (2011b) “Regulatory relationship between tactile sensation at the vermilion of the lips and lip-closing force,” Journal of Oral Rehabilitation. 38 (8) 579-587.
Publisher – Google Scholar
17. Nakatsuka, K., Adachi, T., Kato, T., Murakami, M., Yamada, K. and Masuda, Y. (2011c) “Asymmetric lip-closing forces in children with repaired unilateral cleft lip and/or palate,” Journal of Oral Rehabilitation. 38 (12) 921-928.
Publisher – Google Scholar
18. Posen, A. L. (1976) “The application of quantitative perioral assessment to orthodontic case analysis and treatment planning,” Angle Orthod. 46 (2) 118-143.
Publisher – Google Scholar
19. Thuer, U. and Ingervall, B. (1986) “Pressure from the lips on the teeth and malocclusion,” American Journal of Orthodontics and Dentofacial Orthopedics. 90 (3) 234-242
Publisher – Google Scholar