Introduction
Patients with solid cancers lose weight and have decreased appetite, early saturation and nausea mainly related to the tumour burden (Ravasco et al, 2003), but also correlated to intake deficits (Ravasco et al, 2007). Comparable results are not available in haematological cancers, but at least during the cytotoxic therapy it is the clinical experience, that the nutritional problems are even more pronounced than in patients with solid cancers. In patients with malignant haematological disease with high-dose chemotherapy and often stem-cell transplantation, changes in taste and smell appear with particular difficulty in differentiating sour and bitter (Epstein et al, 2002). In these hyper metabolic cancer patients, protein-intake is important due to gluconeogenesis, with a loss of lean body mass (LBM). This loss of LBM can potentially be reduced by protein supplements as an integrated part of dietary counselling, but it is only shown in patients with colorectal cancer undergoing radiotherapy (Ravasco et al, 2005). However, poor compliance often results in patients not reaching their nutritional goals (Ravasco, 2005), and part of this are taste-related problems. Nutritional supplements are developed in an industrial setting and analysis of taste is very often done in a laboratory by a censoring panel. This setting and these censors are quite different from the patients. Patients with gastro-intestinal cancers seem to prefer fresh-milk-based supplements to UHT milk based (Ultra High Temperature) and fruit juice based, also during chemotherapy. However, vitamins and minerals were added to both the UTH-milk based and the fruit based products, and all were hyperosmolar (Rahemtulla et al, 2005). No similar studies have been published for patients with malignant, haematological diseases.
This study aimed to determine the patients’ preferences for three different ONS including non-vitamin-enriched and freshly made products. We wanted to examine taste perception, and to assess the reproducibility of the taste assessments by means of a Visual Analogue Scale (VAS) in patients with malignant haematological disease.
Methods
VAS (Visual Analogue Scale)
The reproducibility of VAS is relatively well documented in other scientific areas and is described as a valid measure of subjective phenomenon, but carries a phenomenological problem with an underlying acceptance of linearity, which might not be true (Rødbotten, 1997). In this study a unipolar continuous scale was used to evaluate the sensory variables: sweet, sour, bitter, salt, thickness, gritty and metal and the palatability (the ability to drink a glass of the product (150 ml)). All the VAS-scores were performed immediately after tasting, and at the end of the experiment patients rated the three (four) products 1-3(4), as one was repeated.
Selection of Products
Three milk-based products were selected, as these were the three mostly used products in the department: Nutridrik® from Nutricia, Koldskål (RH) from the kitchen in Rigshospitalet and Protin® from Arla. The products had the same flavour, Vanilla and had similar protein content (Nutridrik® 6g/100ml, Protin® 5.7g/100ml and RH 5 g/100ml). Nutridrik® is a UHT milk based, hyperosmolar product from Nutricia with added vitamins and minerals with an osmolarity of 450 mOsm/l (in 100 ml: 630 kJ, 18.4 g carbohydrate, 5.8 g fat). RH is a fresh cold buttermilk based product with eggs made in the Kitchen on Rigshospitalet from day to day. The recipe for one litre is: Junket 3 dl, buttermilk 6 dl, egg-yolk 80 g, sugar 45 g, and the osmolarity is 653 mOsm/l. Junket, egg and buttermilk is whippet, sugar is added and the taste is adjusted with vanilla sugar and lemon (in 100 ml: 356 kJ, 9.3 g carbohydrate, 3.1 g fat). Protin® is a fresh milk based product with added milk-proteins from the diary, Arla with a shelf life of 10 days (open 3 days), osmolarity 718 mOsm/l (in 100 ml: 540 kJ, 12 g carbohydtate, 6.3 g fat)..
Taste samples
The products were served in a plastic cup (4 ml) at room temperature in a random rotating order on the same day. The patients were blinded to the products. The samples were served according to a preformed protocol with random allocation of the drinks, and the repeated drink in a random position in the sequence. One of the samples was repeated in every experiment to quantitate reproducibility.
Viscosity
The viscosity was determined by the Laboratory of Rheology and Texture, The department of Food Technology, The Technical University of Denmark by the shear stress/shear rate (Pa s). Shear stress is the force that moves the liquid, and shear rate (1/s) is the velocity gradient.
Subjects
Forty-one patients from the haematological clinic in Rigshospitalet participated in the study (table 1). Patients were asked for participating consecutively on rounds if they fulfilled the inclusion criteria. Inclusion criteria: patients in treatment in one of the four haematological units, no distinction for cancer type, gender or type of treatment. The time interval from the last chemotherapy or radiation therapy varied from two weeks to two months. All the patients had severe eating problems at the time of investigation, and all had mucositis visually diagnosed. All patients were of legal age and mentally able to understand written and verbal information. Exclusion criteria: use of parenteral nutrition or tube feeding, lack of ability to communicate and/or cooperate. All patients gave written consent.
The protocol was approved by the regional ethical committee.
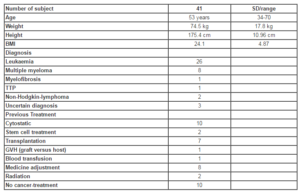
Table 1: Baseline characteristics for 41 patients with haematological malignant disease and mucositis.
Results
VAS
The patients’ median and average VAS scores for the 3 drinks were similar (table 2),
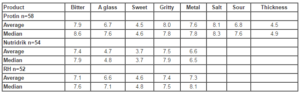
Table 2: Average and median score of the sensory variables for Protin, RH and Nutridrik. The numbers are in cm measured on a 10 cm VAS scale. Sensory parameters 0: Too much of the variable, 10: Too little of the variable. Drink a glass 0: Not alt all, 10: No problem. In 41 patients with haematological malignant disease
without significant difference between the three products concerning the sensory variables sour and sweet (table 3). There was significant difference concerning the sensory variables of the three products (table 3).
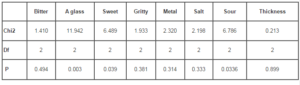
Table 3: Result of Kruskal-Wallis test of the sensory variables for the three protein containing drinks in 41 patients with malignant haematological disease
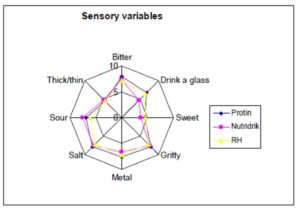
The taste characteristics are shown in figure 1. The differences in sweet, sour and sensory variables are illustrated. The VAS evaluation of the three products as a hole was not markedly different; their spider web had similar looks. We found no systematic relation between the VAS evaluations and the time passed from the preceding therapeutic session.
Figure 1: Nutritional supplements – Taste preferences divided in categories in patients with malignant haematological disease during active treatment with chemotherapy. Spider web of the sensory variables (Bitter, a glass, gritty, metal, salt, sour, sweet and thickness) for three products (Protin, Nutridrik and RH (= a fresh cold buttermilk based product produced in the hospital) in 41 patients with haematological malignant disease. Sensory parameters: 0: Too much of the sensory variable. 10: Too little of the sensory variable. Acceptability – Drink a glass: 0: Not at all 10: No problem
The sensory differences of the three products
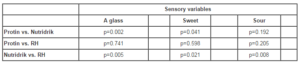
The results were detailed further (table 4). The patients judged that Nutridrik® had a significant sweeter taste than Protin® (p=0.041) and RH (p=0.021); the patients liked Protin® (p=0.002) and RH (p=0.005) significantly better than Nutridrik®. The patients judged that RH (p=0.008) had a significantly more sour taste than Nutridrik®. No significant differences were found between Protin® and RH with regard to any of the sensory variables.
Table 4: Result of Mann-Whitney test for sour, sweet and the ability to ingest a glass of 150 ml of the drink in 41 patients with haematological malignant disease.
Preferences (which drink do you prefer?)
The patients had a significantly higher preference for Protin® compared to RH and especially to Nutridrik®: Protin® vs. Nutridrik® (p< 0.001), Protin® vs. RH (p=0.049) and RH vs. Nutridrik® (p=0.008).
Ability to drink 150 ml (how difficult is it to drink one glass = 150 ml?)
Patients VAS-scored a significantly higher ability to drink 150 ml of Protin® and RH compared to Nutridrik® (table 4).
Reproducibility
Identical (+/- 10% in cm) VAS-score was seen in 39 of the 41 patients (95%), when blindly testing the same sample twice in random order mixed-in with the other samples.
Viscosity
The difference between the fresh milk products (Protin® and RH) and the commercial (Nutridrik®) was marked (Table 5 and fig 2).
Table 5: Viscosity measurements in milk-based oral, protein-enriched supplements. Nutridrik is a commercial drink with added minerals and vitamins, Protin is milk with added whey-protein and RH is buttermilk with eggs. The trendlines are shown in fig. 2. n and m are the indices of the powerlaw model with m as the general viscosity. N<1 means that the liquid becomes more thick when stirred.
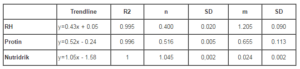
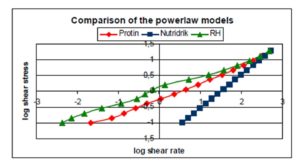
Figure 2: Nutritional supplements — Viscosity determinations. Shear stress (Pa) is the force that moves the liquid. Shear rate (1/s) is the velocity gradient. The difference in profile is marked between the commercial, milk-based Nutridrink and the fresh milk based drinks, Protin and RH.
Statistics
As results were distributed very skew, non-parametric methods were applied, Wilcoxon-, Mann-Whitney rank-sum tests, and Kruskal-Wallis test.
Discussion
Dysgeusia associated with weight loss due to lack of appetite and altered eating pattern influence the patient’s Quality of life. Dysgeusia is caused by many factors, and simple studies of individual taste sensitivity using single taste stimuli (sweet, sour, salt, umami or bitter) are not considered predictive of dysgeusia nor of food aversions (Settle et al, 1978). The patients’ preferences for fresh (no UHT) milk-based products (Protin and RH) are similar to results found in other studies. Rahemtulla et al (2005) found no significant difference in preference for nutritional supplement due to disease or cytostatic treatment of 47 patients with gastrointestinal cancer and 47 healthy controls. Both groups had a preference for “Calshake”, a fresh milk based product (No UHT) with strawberry flavour. Comparable results were reported by Darmon et al (2008) testing 109 malnourished in-patients, who preferred milk-based supplements to sweet and salty fruit-juice typed products. In a study of 60 patients with colorectal cancer using single taste-stimuli, Kucz et al found a reduced sensitivity of taste compared to healthy controls (Kucz et al, 2008). This would indicate that cancer patients might prefer strongly flavoured foods. However, our results did not confirm such a hypothesis. Pelvic radiotherapy did not markedly affect supplement preference in a case-control study with healthy controls, but only 28% of the cancer patients received concomitant chemotherapy (McGough et al, 2006). In our setting, we found no systematic influence of the time-interval from the last chemotherapy or radiation therapy, but all the patients had mucositis. Even though individual differences in taste perception are many and complicated (Stevens, 1996), and despite the complex effects of disease, dissemination of disease, and treatment (Hutton et al, 2007), results seem to have some uniform directions. Fresh, milk based products seem to have a higher acceptability, but agreement is not complete. Several explanations might contribute. We know that hyperosmolarity is a problem for patients with mucositis, but all three drinks in our experiment were considerably hyperosmolar, making this factor an unlikely explanation. Texture was also markedly different (fig 2). Whether this is a determining factor or not cannot be answered with our present knowledge, but the enriched milk and the buttermilk-drink were very similar, and they were both evaluated as positive by the patients. Nutridrink showed different results, and was evaluated very negative. This may indicate that texture could be part of an explanation. We tried to interview the patients for details related to their own scoring, but gave it up, as most patients felt too tired after the testing sessions. Smell and viscosity as well as other textural variables could be factors involved.
The advantages of the commercial “full-nutritional” drinks are their content of micronutrients, their very long shelf-life, and the control procedures related to the manufacturing. The micronutrients might well be the reason for the reduced palatability, but future studies are needed to elucidate this.
All the published studies about taste disturbances in patients with malignant diseases are single meal tests. In the future, we would need long time studies using the results from the meal-studies to elucidate whether there are positive effects on nutritional status during the course of treatment, as compliance in the long run is determining the clinical value. Weight as well as body composition and quality of life should be used as outcome variables.
Conclusion
This study gives an indication of patients’ preference with significant higher preference and palatability for fresh milk products than a commercial, milk based product. However, the basic sensory parameters studied with VAS gave no clear distinction between the three products, and the underlying basis for the preference is not obvious, and merits further investigations. The used test-method was well functioning with a very high reproducibility-rate.
Acknowledgement
We are grateful for the determinations of viscosity by Nancy Kjøbæk, Laboratory of Rheology and Texture, The Department of Food Technology, The Technical University of Denmark, Søltofts Plads, Building 227, 2800 Lyngby, Denmark.
No conflicts of interest
Running head: taste preferences in cancer
References
1. Darmon, P., Karsegard, V.L., Nardo, P., Dupertuis, Y.M. and Pichard, C. (2008) “Oral nutritional supplements and taste preferences: 545 days of clinical testing in malnourished in-patients.” Clin Nutr27:660-665.
Publisher – Google Scholar
2. Epstein, J.B., Phillips, N., Parry, J., Epstein, M., Neville, T. and Stevenson-Moore, P. (2002) “Quality of life, taste, olfactory and oral function following high-dose chemotherapy and allogeneic haematopoietic cell transplantation.” Bone Marrow Transplant 30:785-792.
3. Hutton, J.L., Baracos, V.E. and Wismer, W.V. (2007) “Chemosensory dysfunction id a primary factor in the evolution of declining nutritional status and quality of life in patients with advanced cancer.” J Pain Symptom Management 33:156-165.
Publisher – Google Scholar
4. Kucz, K., Maluck, S., Kohl, O., Wiese, M., Hanrider, D. and Weimann, A. (2008) „Taste perception and nutritional status of colorectal cancer patients under chemotherapy. Clin Nutr 3/suppl 1;100 (abstract).
5. McGough, C., Peacock, N., Hackett, C., Baldwin, C., Norman, A., Frost, G., Blake, P., Tait, D., Khoo, V., Harrington, K., Whelan, K., Jervoise, H. and Andreyev, N. (2006) “Taste preferences for oral nutrition supplements in patients before and after pelvic radiotherapy: a double-blind controlled study.” Clin Nutr 25:906-912.
Publisher – Google Scholar
6. Rahemtulla, Z., Baldwin, C., Spiro, A., McGough, C., Norman, A.R., Frost, G., Cunningham, D., Jervoise, H and Andreyev, N.(2005) “The palatability of milk-based and non-milk-based nutritional supplements in gastrointestinal cancer and the effect of chemotherapy.” Clin Nutr 24:1029-1037.
Publisher – Google Scholar
7. Ravasco, P., Monteiro-Grillo, I., Vidal, P.M. and Camilo, M.E. (2003) “Nutritional deterioration in cancer: The role of disease and diet.” Clin Oncol (R Coll Radiol) 15:443-450.
Publisher – Google Scholar
8. Ravasco, P. (2005) “Aspects of taste and compliance in patients with cancer.” Eur J Oncol Nursing 9(suppl 2):S84-91.
Publisher – Google Scholar
9. Ravasco, P., Monteiro-Grillo, I., Vidal, P.M. and Camilo, M.E. (2005) “Dietary counselling improves patient outcomes: A prospective, randomized, controlled trial in colorectal cancer patients undergoing radiotherapy.” J Clin Oncol 23:1431-1438.
Publisher – Google Scholar
10. Ravasco, P., Grillo, I.M. and Camillo, M. (2007) “Cancer wasting and quality of life react to early individualized nutritional counselling.” Clin Nutr 26:7-15.
Publisher – Google Scholar
11. Rødbotten, M. (1997) ”Kap.7: Metoder i sensorisk analyse” In ”sensorisk analyse — Bedømmelse af næringsmidler” Sensorisk studiegruppe. 2. ed., Universitetsforlaget Oslo, Norway
12. Settle, R.G., Quinn, M.R. and Kare, M.R. (1978) “Evaluation of Cancer Patients, including Interim Report 1 on Task 1 and 2 and analysis from Task 4. Contract no. NOl-CP-6579l”. Report of the August 4, 1978, Meeting of Gustatory, Philadelphia: Monell chemical Senses Centre, University of Pennsylvania.
13. Stevens, D.A. (1996) “Individual differences in taste perception.” Food Chemistry 56:303-311.
Publisher – Google Scholar